The Bookout Center
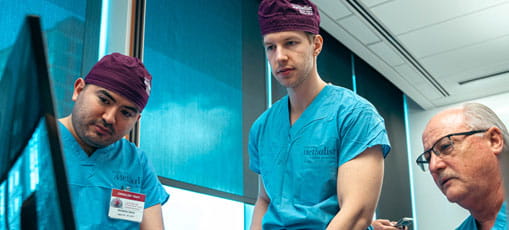
Shaping The Next Generation
Learn more about the MITIE-hosted DeBakey Heart & Vascular Center boot camp which helped fellows and faculty establish a foundation of success
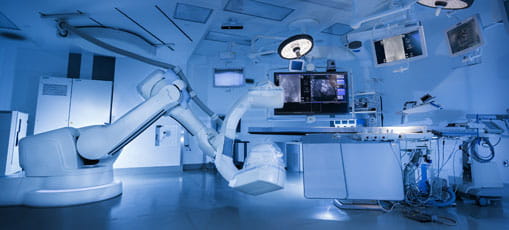
Simulation Center Tour
You can now explore all three floors of the Sim Center at MITIE, virtually. The first facility of its kind, MITIE now encompasses 35,000 square feet of research and training space.
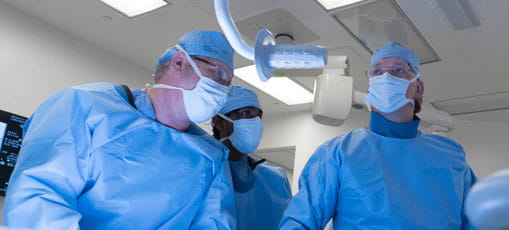
World Class Resources
MITIE has become a center for innovative ideas and technological advances that offers an extensive array of resources for training, research and device development.
Function and Purpose
The MITIE research and training spaces are housed under one roof. This enables the logical, progressive development of collaborative research and training efforts. The learning process begins with the development of new technology or procedural techniques by scientists and physicians working in the research core of MITIE. These advances evolve through the use of a simulated patient care environment. Once the efficacy of a technology or procedure is proven, it can be disseminated to practicing physicians in the MITIE training area and MedPresence room.
Goals
- Develop novel technologies to enable less invasive medical care.
- Demonstrate cutting-edge techniques via live audio and video conferencing within all Houston Methodist procedure areas.
- Influence local, regional, national and international health care professionals and providers.
Objectives
- Train physicians in procedural skills across multiple specialties.
- Conduct research on the metrics of skills acquisition.
- Enhance patient safety using high fidelity simulation training.
Approach
- Practicing physicians can access all components under one roof.
- Remote telementoring uses audiovisual conferencing via wearable technology.
- Image guidance enhances procedural accuracy.
- Robotics improve the efficacy and outcomes of minimally invasive procedures.
35,000
Square Feet of Research and Training Space
3,978
Learners in 2023
Interested in hosting an event at MITIE?
Please contact us at mitieevents@houstonmethodist.org or 888.648.4389.
A member of our team will reach out to you within 24-48 hours to discuss your requirements and ensure a successful event.

